Contact us on 0800 612 4812
10% off your first order Sign up NOW!
Hyperhidrosis: what it is and how to treat it

Why do I sweat?
The bigger question is… who doesn’t?
Let’s face it; we all do at some point or another to varying levels! It is in fact a perfectly normal part of being human and nothing to be ashamed of.
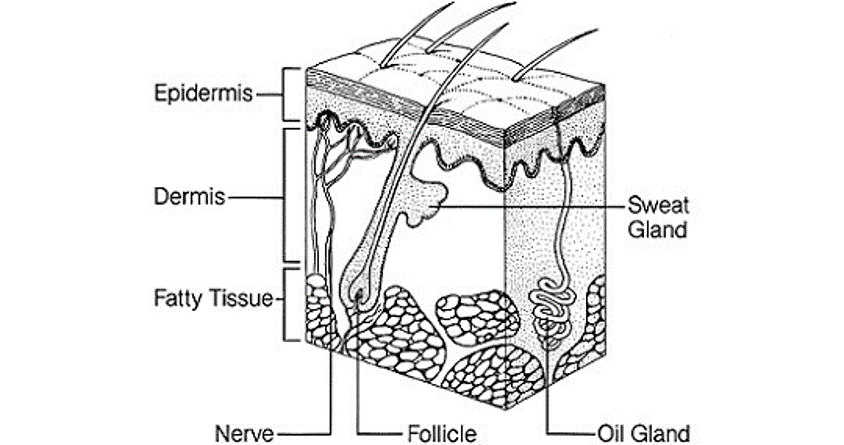
Put simply, we sweat primarily to control body temperature. We have sweat glands all over our body, but they are most numerous on the forehead, armpits, palms of hands and soles of feet. Sweat is mainly water with some salt content, when we sweat the water in the sweat evaporates and cools the surface of the skin. Sweat itself hardly ‘smells’ at all, but when the bacteria that lives naturally on our skin begins to ‘eat’ some of the by-products that sweat produces, it results in creating and releasing what we know as ‘body odour’ – you can find out more about body odour here.
Now more than ever we live in a world that promotes good health and personal hygiene, so when we cannot control or improve that which is naturally produced with washing and off the shelf antiperspirants we have to stop and consider whether we have ‘regular sweating’ or whether a condition known as Hyperhidrosis may be the cause?
What is Hyperhidrosis?
Well, Hyperhidrosis is a disabling medical condition that affects the bodies’ sweating mechanism causing a severe over-reaction of the sympathetic nervous system resulting in heavy, excessive perspiration. Put simply, Hyperhidrosis is excessive sweating either all the time or at times when the body does not need to sweat, and is often devastating to the sufferer.
There are two types of Hyperhidrosis:
• Primary
• Secondary
What is Primary Hyperhidrosis?
The medical profession do not fully understand the reasons or triggers for Hyperhidrosis occurring in patients, but Primary Hyperhidrosis is defined as over activity in the sympathetic nervous system, specifically, it is the Thoracic Sympathetic Ganglion Chain, which controls the release of Acetylcholine. Acetylcholine (ACH) is an electrically charged neurotransmitter produced by the body that stimulates the gland, creating production of sweat. Hyperhidrosis patients experience an over-reaction of this process which results in excess sweating.
In easier terminology, in non-Hyperhidrosis sufferers, the brain sends signals to the nerves around the sweat glands which triggers the opening and secretion of sweat only at times when it is needed.
For example, if the body is hot it will sweat to cool itself down (this process is called Thermoregulation). In the case of a patient who has Hyperhidrosis, these signals are sent continuously, and so sweat glands react constantly and at times when the body is not in need of sweat production for thermoregulation.
What is Secondary Hyperhidrosis?
Secondary Hyperhidrosis is caused by many factors including, obesity, poor diet, menopause, anxiety and stress. It is no less distressing but may be caused by lifestyle factors as opposed to genetic or physiological responses.
Why me?
Despite what you may think, it’s not just you. If you had an honest and frank conversation with friends we feel certain that you would be surprised at how many of them suffer with sweat problems without you even knowing.
Hyperhidrosis affects approximately 4% of the population, or around 2.5 million people in the UK, so it is in fact more common than most people believe. Sufferers tend to go to great lengths to hide their condition and there is a far wider section of the population who suffer with problematic sweat and / or odour, but do not necessarily have Hyperhidrosis.
The stigma surrounding excessive sweating is often the most debilitating part of the condition. The anxiety, depression, the lack of confidence, ridicule and often the withdrawal from social situations that the sufferer may experience as a result of it can be far worse than the sweating itself. This is particularly true with younger teenage patients, who frankly already have enough to deal with. Although rare in pre-pubescent children, cases of Hyperhidrosis have been recorded in people as young as 5 years old. The constant wetness can also cause other skin conditions which are further aggravated by the sweating.
Whilst there is no cure, the good news is it can be treated, to reduce and improve the levels of sweat, and it is important to bear in mind that you are not alone.
What areas are affected by Hyperhidrosis?
Hyperhidrosis can affect any area of the body, but some areas are affected more commonly than others. The most common would be hands and feet, closely followed by underarms, face and neck, groin and torso.
Axillae Hyperhidrosis – excessive underarm sweating
Palmer Hyperhidrosis – excessively sweating palms
Plantar Hyperhidrosis – excessively sweaty feet
Some less commonly affected areas include:
Cranial Hyperhidrosis – Excessive head sweating
Facial Hyperhidrosis – Excessive facial sweating
Torso Hyperhidrosis – Excessive bodily sweating (including the groin and buttocks).
What treatment is there for excessive sweating (Hyperhidrosis)?
The first step is to recognise and understand the underlying cause of the condition, the information outlined already should go a long way towards helping with that.
As already mentioned the causes of Hyperhidrosis vary, they can be from genetic or hereditary sources, or caused by physiological triggers (weight, diet, hormonal changes for example) or psychological conditions such as anxiety or stress. Regardless of the cause, there is very little than can cure the condition, but thankfully there are products and treatments available that will at least control the problem. Many patients are lucky in that the severity of the condition reduces or even stops completely with age, but for others Hyperhidrosis is a lifelong battle.
In the first instance
When symptoms are present, the first course of action is generally use of a topical high strength antiperspirant, such as Perspi-Guard® Maximum Strength Antiperspirant. There are several other products on the market with varying degrees of efficacy and suitability, but Perspi-Guard® is very well received by most and is available in several formats including spray, roll-on and wipes. Most other high strength antiperspirants have been created with high percentages of active ingredients which can be abrasive to skin and therefore unusable for many, whereas Perspi-Guard® products can be used by all whether you suffer from excessive sweating or not!
Perspi-Guard® Maximum Strength has been formulated and engineered with significantly lower levels of active ingredients to provide a clinically proven level of protection that enables most users to only require application once or twice per week to maintain dryness, but doesn’t prevent more frequent application if required. Perspi-Guard® can be used on the underarms, hands and even the feet but it is important to understand that antiperspirants are mainly intended for the underarms.
Did you know…That in addition to your statutory rights, Perspi-Guard® offer a 30 day no-quibble Money-Back Guarantee on all products! That’s how confident we are in the Perspi-Guard® range.
If you find any Perspi-Guard® product is non-responsive and would like to return it, contact us straight away. We have found that in most cases, a simple call to Customer Services can result in much better results, as it is often the case that the product has been applied incorrectly.
In the unlikely event of you still being unhappy after discussing your purchase with us, you may request to return it within 30 days of date of original delivery. Once your return is received, a full refund of purchase price of your order will be paid within 14 days.
Thankfully, antiperspirants are the easiest to apply, least expensive and invasive treatment option available to suffers and most will respond to topical applications. If you find that high strength antiperspirants do not control the sweating, then there are other options available. These treatment options are progressively more intensive and invasive but there are non-invasive treatments that will offer great results for hyperhidrosis patients.
At this point you should consult your GP or Healthcare professional for further advice. They will most likely refer you to a dermatologist for alternative treatment.
Iontophoresis – a non-invasive treatment for Hyperhidrosis
Should an antiperspirant treatment not be suitable for you then there are several other treatment options available. Drawing on many years’ experience within this area, our recommendation would be to explore a treatment called Iontophoresis.
It is an increasingly common treatment option used with excellent results in hospitals, clinics and at home. Iontophoresis involves passing regulated and controlled mild electrical current into the body in the area that one is suffering with Hyperhidrosis.
Over the course a few short treatments using only tap water, the sweating in the area stops. This treatment option has been around for decades and it extremely popular in Europe and over recent years has gained traction in UK NHS hospitals, fast becoming the preferred option for Hyperhidrosis treatment. Results can vary from patient to patient but in general results from the treatment are excellent and can last several weeks before a single 20 minute ‘top up’ treatment is required. Success rates for Palmer (hand) and Plantar (foot) Hyperhidrosis patients are in the high 98% area.
There are several high-quality manufacturers on the market such as Hidrex® and Idromed®. These manufacturers provided high quality machines that are certified and CE marked. This is important as there are overseas producers who are selling illegal units cheap. These can be dangerous and are not tested or legal to use in the UK or the EU. For more information regarding Iontophoresis treatments for Hyperhidrosis, please visit IontoCentre.
Medication is another option
If the non-invasive options mentioned above do not work then you can move your treatment plan on to try alternative products and medications.
Your GP or Dermatologist will advise you further on the range of prescribed medications you can use to control Hyperhidrosis. There are some very effective treatment options available, so it is important to not to lose hope of ending your excessive sweating. Some medications can be used in conjunction with Iontophoresis. A major drawback of oral medications for Hyperhidrosis is that there can be systemic effects. This is where you take a medicine to stop your sweating, but you also encounter dry mouth and eyes for example.
Iontophoresis can position medications where needed without systemic effects.
What about Botox?
Botox is also an effective method of treatment particularly in the underarm region, but also for the palms and the feet. There is a cost issue involved with Botox treatments and patients may require several treatments per year.
Most NHS clinics do not have the budget capacity to offer Botox but there are private clinics who will offer treatment courses if you are willing to pay. A high-quality advanced Iontophoresis machine will cost around £550 and last for 15+years and equates to about 6 months of injections so there is a big price difference in these treatments.
What about surgery?
Medical procedures such as ETS surgery can cure palmer hyperhidrosis, but many people are hesitant to undergo this possibly risky and serious operation, preferring to control the condition instead using non-invasive measures.
A possible side effect of ETS surgery is compensatory sweating elsewhere on the body, for example the surgical procedure halts sweating of the palms but can cause excessive sweating on the chest or groin or face. Again, you doctor will advise you on this.
There have been many reported cases of patients who undergo this surgical procedure with great results initially only to find that sweating appears elsewhere on the body.
Why do I sweat?
The bigger question is… who doesn’t?
Let’s face it; we all do at some point or another to varying levels! It is in fact a perfectly normal part of being human and nothing to be ashamed of.
Put simply, we sweat primarily to control body temperature. We have sweat glands all over our body, but they are most numerous on the forehead, armpits, palms of hands and soles of feet. Sweat is mainly water with some salt content, when we sweat the water in the sweat evaporates and cools the surface of the skin. Sweat itself hardly ‘smells’ at all, but when the bacteria that lives naturally on our skin begins to ‘eat’ some of the by-products that sweat produces, it results in creating and releasing what we know as ‘body odour’ – you can find out more about body odour here.
Now more than ever we live in a world that promotes good health and personal hygiene, so when we cannot control or improve that which is naturally produced with washing and off the shelf antiperspirants we have to stop and consider whether we have ‘regular sweating’ or whether a condition known as Hyperhidrosis may be the cause?
What is Hyperhidrosis?
Well, Hyperhidrosis is a disabling medical condition that affects the bodies’ sweating mechanism causing a severe over-reaction of the sympathetic nervous system resulting in heavy, excessive perspiration.
Put simply, Hyperhidrosis is excessive sweating either all the time or at times when the body does not need to sweat, and is often devastating to the sufferer.
There are two types of Hyperhidrosis:
• Primary
• Secondary
What is Primary Hyperhidrosis?
The medical profession do not fully understand the reasons or triggers for Hyperhidrosis occurring in patients, but Primary Hyperhidrosis is defined as over activity in the sympathetic nervous system, specifically, it is the Thoracic Sympathetic Ganglion Chain, which controls the release of Acetylcholine. Acetylcholine (ACH) is an electrically charged neurotransmitter produced by the body that stimulates the gland, creating production of sweat.
Hyperhidrosis patients experience an over-reaction of this process which results in excess sweating.
In easier terminology, in non-Hyperhidrosis sufferers, the brain sends signals to the nerves around the sweat glands which triggers the opening and secretion of sweat only at times when it is needed.
For example, if the body is hot it will sweat to cool itself down (this process is called Thermoregulation). In the case of a patient who has Hyperhidrosis, these signals are sent continuously, and so sweat glands react constantly and at times when the body is not in need of sweat production for thermoregulation.
What is Secondary Hyperhidrosis?
Secondary Hyperhidrosis is caused by many factors including, obesity, poor diet, menopause, anxiety and stress.
It is no less distressing but may be caused by lifestyle factors as opposed to genetic or physiological responses.
Why me?
Despite what you may think, it’s not just you. If you had an honest and frank conversation with friends we feel certain that you would be surprised at how many of them suffer with sweat problems without you even knowing.
Hyperhidrosis affects approximately 4% of the population, or around 2.5 million people in the UK, so it is in fact more common than most people believe. Sufferers tend to go to great lengths to hide their condition and there is a far wider section of the population who suffer with problematic sweat and / or odour, but do not necessarily have Hyperhidrosis.
The stigma surrounding excessive sweating is often the most debilitating part of the condition. The anxiety, depression, the lack of confidence, ridicule and often the withdrawal from social situations that the sufferer may experience as a result of it can be far worse than the sweating itself. This is particularly true with younger teenage patients, who frankly already have enough to deal with. Although rare in pre-pubescent children, cases of Hyperhidrosis have been recorded in people as young as 5 years old. The constant wetness can also cause other skin conditions which are further aggravated by the sweating.
Whilst there is no cure, the good news is it can be treated, to reduce and improve the levels of sweat, and it is important to bear in mind that you are not alone.
What areas are affected by Hyperhidrosis?
Hyperhidrosis can affect any area of the body, but some areas are affected more commonly than others.
The most common would be hands and feet, closely followed by underarms, face and neck, groin and torso.
Axillae Hyperhidrosis – excessive underarm sweating
Palmer Hyperhidrosis – excessively sweating palms
Plantar Hyperhidrosis – excessively sweaty feet
Some less commonly affected areas include:
Cranial Hyperhidrosis – Excessive head sweating
Facial Hyperhidrosis – Excessive facial sweating
Torso Hyperhidrosis – Excessive bodily sweating
(including the groin and buttocks)
What treatment is there for excessive sweating (Hyperhidrosis)?
The first step is to recognise and understand the underlying cause of the condition, the information outlined already should go a long way towards helping with that.
As already mentioned the causes of Hyperhidrosis vary, they can be from genetic or hereditary sources, or caused by physiological triggers (weight, diet, hormonal changes for example) or psychological conditions such as anxiety or stress.
Regardless of the cause, there is very little than can cure the condition, but thankfully there are products and treatments available that will at least control the problem.
Many patients are lucky in that the severity of the condition reduces or even stops completely with age, but for others Hyperhidrosis is a lifelong battle.
In the first instance
When symptoms are present, the first course of action is generally use of a topical high strength antiperspirant, such as Perspi-Guard® Maximum Strength Antiperspirant. There are several other products on the market with varying degrees of efficacy and suitability, but Perspi-Guard® is very well received by most and is available in several formats including spray, roll-on and wipes.
Most other high strength antiperspirants have been created with high percentages of active ingredients which can be abrasive to skin and therefore unusable for many, whereas Perspi-Guard® products can be used by all whether you suffer from excessive sweating or not!
Perspi-Guard® Maximum Strength has been formulated and engineered with significantly lower levels of active ingredients to provide a clinically proven level of protection that enables most users to only require application once or twice per week to maintain dryness, but doesn’t prevent more frequent application if required. Perspi-Guard® can be used on the underarms, hands and even the feet but it is important to understand that antiperspirants are mainly intended for the underarms.
Did you know…That in addition to your statutory rights, Perspi-Guard® offer a 30 day no-quibble Money-Back Guarantee on all products! That’s how confident we are in the Perspi-Guard® range.
If you find any Perspi-Guard® product is non-responsive and would like to return it, contact us straight away. We have found that in most cases, a simple call to Customer Services can result in much better results, as it is often the case that the product has been applied incorrectly.
In the unlikely event of you still being unhappy after discussing your purchase with us, you may request to return it within 30 days of date of original delivery. Once your return is received, a full refund of purchase price of your order will be paid within 14 days.
Thankfully, antiperspirants are the easiest to apply, least expensive and invasive treatment option available to suffers and most will respond to topical applications. If you find that high strength antiperspirants do not control the sweating, then there are other options available.
These treatment options are progressively more intensive and invasive but there are non-invasive treatments that will offer great results for hyperhidrosis patients.
At this point you should consult your GP or Healthcare professional for further advice. They will most likely refer you to a dermatologist for alternative treatment.
Iontophoresis – a non-invasive treatment for Hyperhidrosis
Should an antiperspirant treatment not be suitable for you then there are several other treatment options available.
Drawing on many years’ experience within this area, our recommendation would be to explore a treatment called Iontophoresis.
It is an increasingly common treatment option used with excellent results in hospitals, clinics and at home.
Iontophoresis involves passing regulated and controlled mild electrical current into the body in the area that one is suffering with Hyperhidrosis.
Over the course a few short treatments using only tap water, the sweating in the area stops.
This treatment option has been around for decades and it extremely popular in Europe and over recent years has gained traction in UK NHS hospitals, fast becoming the preferred option for Hyperhidrosis treatment.
Results can vary from patient to patient but in general results from the treatment are excellent and can last several weeks before a single 20 minute ‘top up’ treatment is required.
Success rates for Palmer (hand) and Plantar (foot) Hyperhidrosis patients are in the high 98% area.
There are several high-quality manufacturers on the market such as Hidrex® and Idromed®. These manufacturers provided high quality machines that are certified and CE marked.
This is important as there are overseas producers who are selling illegal units cheap. These can be dangerous and are not tested or legal to use in the UK or the EU.
For more information regarding Iontophoresis treatments for Hyperhidrosis, please visit IontoCentre.
Medication is another option
If the non-invasive options mentioned above do not work then you can move your treatment plan on to try alternative products and medications.
Your GP or Dermatologist will advise you further on the range of prescribed medications you can use to control Hyperhidrosis. There are some very effective treatment options available, so it is important to not to lose hope of ending your excessive sweating. Some medications can be used in conjunction with Iontophoresis. A major drawback of oral medications for Hyperhidrosis is that there can be systemic effects. This is where you take a medicine to stop your sweating, but you also encounter dry mouth and eyes for example.
Iontophoresis can position medications where needed without systemic effects.
What about Botox?
Botox is also an effective method of treatment particularly in the underarm region, but also for the palms and the feet. There is a cost issue involved with Botox treatments and patients may require several treatments per year.
Most NHS clinics do not have the budget capacity to offer Botox but there are private clinics who will offer treatment courses if you are willing to pay. A high-quality advanced Iontophoresis machine will cost around £550 and last for 15+years and equates to about 6 months of injections so there is a big price difference in these treatments.
Medical procedures such as ETS surgery can cure palmer hyperhidrosis, but many people are hesitant to undergo this possibly risky and serious operation, preferring to control the condition instead using non-invasive measures.
A possible side effect of ETS surgery is compensatory sweating elsewhere on the body, for example the surgical procedure halts sweating of the palms but can cause excessive sweating on the chest or groin or face. Again, you doctor will advise you on this.
There have been many reported cases of patients who undergo this surgical procedure with great results initially only to find that sweating appears elsewhere on the body.
 Store Finder
Store Finder